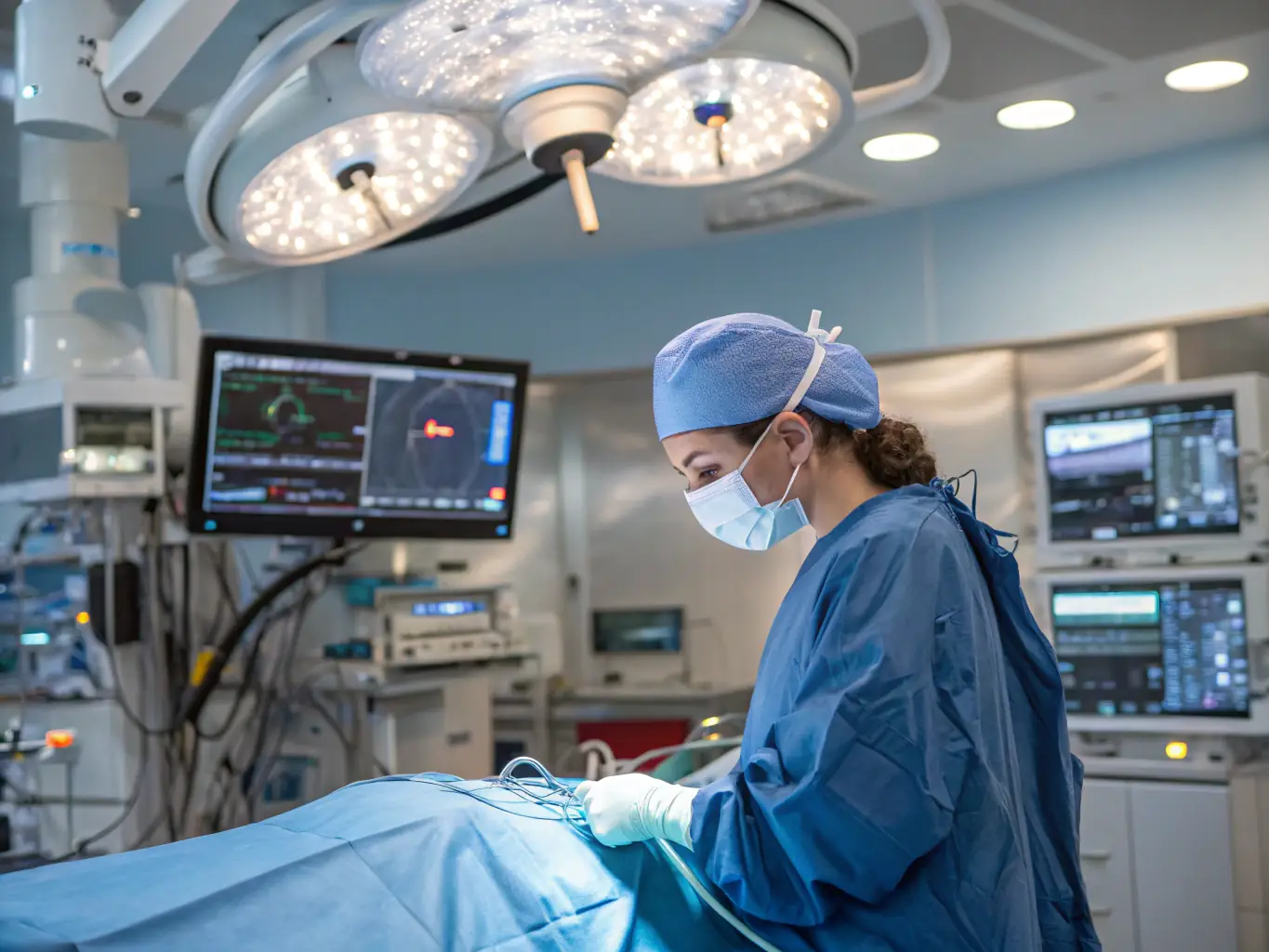
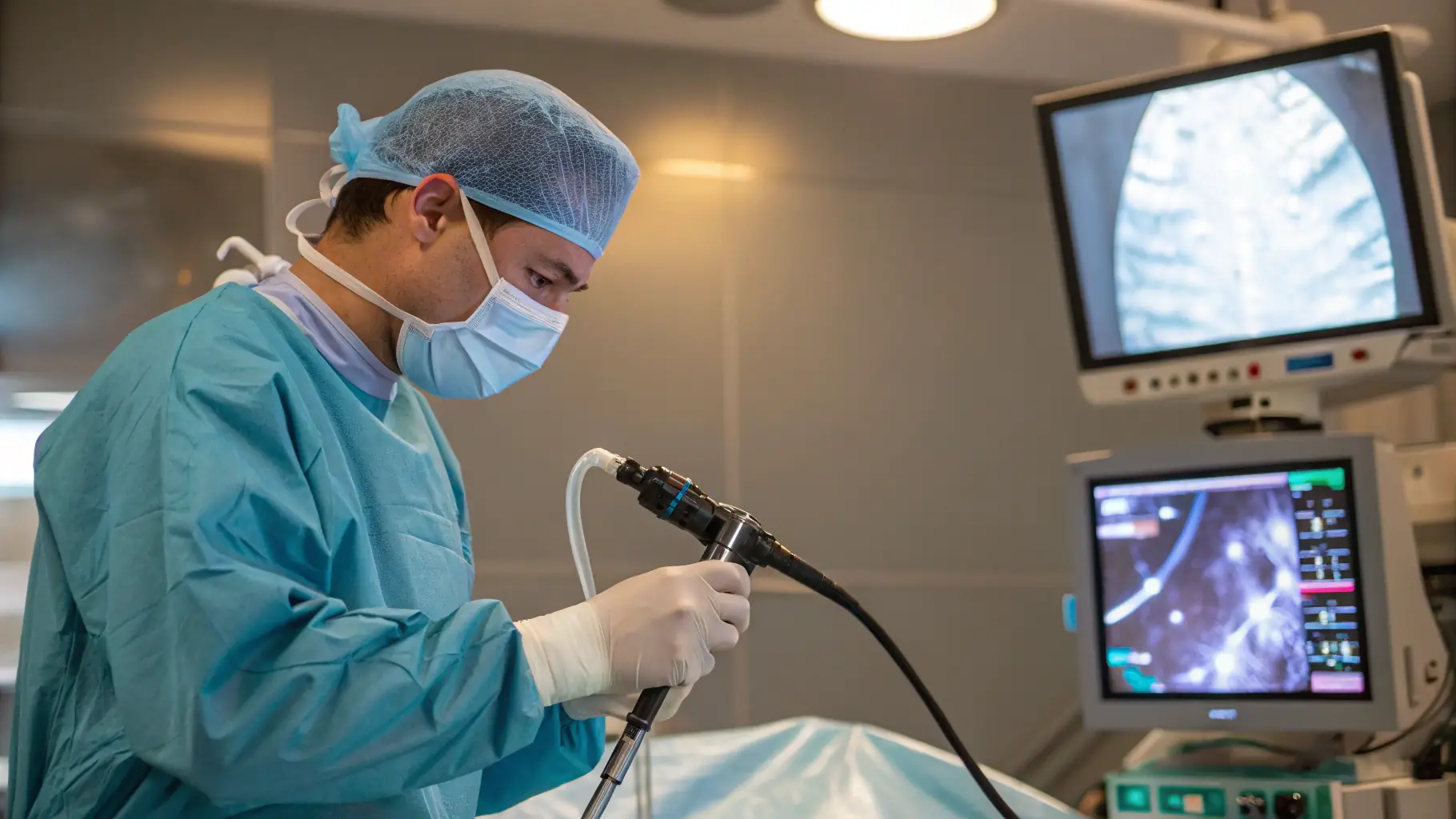
Bariatric surgery refers to various surgical procedures that alter your digestive system to promote weight loss. Read more here.
Bariatric surgery has become one of the most effective long-term solutions for severe obesity, with studies showing it can help patients lose 50-80% of their excess weight and maintain this loss for over a decade (1). But what exactly does this life-changing procedure entail?
Understanding Bariatric Surgery
Bariatric surgery refers to various surgical procedures that alter your digestive system to promote weight loss. These operations work through two primary mechanisms:
Restriction – Reducing stomach size to limit food intake
Malabsorption – Bypassing parts of the small intestine to decrease calorie absorption
According to the American Society for Metabolic and Bariatric Surgery (ASMBS), these procedures are typically recommended for:
Individuals with a BMI ≥40
Those with BMI ≥35 who have obesity-related conditions like:
Type 2 diabetes
Hypertension
Sleep apnea
Severe joint problems (2)
The 4 Main Types of Bariatric Surgery
1. Gastric Sleeve (Sleeve Gastrectomy)
How it works: Surgeons remove about 80% of the stomach, leaving a banana-shaped “sleeve”
Pros:
No intestinal rerouting
Lower risk of nutritional deficiencies
Effective for most patients (50-60% excess weight loss)
Cons:
Irreversible
May worsen acid reflux
Ideal for: First-time patients with BMI 35-50
2. Gastric Bypass (Roux-en-Y)
How it works: Creates a small stomach pouch and reroutes the small intestine
Pros:
Faster initial weight loss
Excellent for diabetes remission
Long-term success (60-70% excess weight loss)
Cons:
More complex procedure
Higher risk of dumping syndrome
Ideal for: Patients with severe GERD or type 2 diabetes
3. Adjustable Gastric Band
How it works: Places an inflatable silicone band around the upper stomach
Pros:
Reversible
No cutting/stapling of stomach
Cons:
Lower weight loss results (40-50%)
Frequent follow-ups needed for adjustments
Ideal for: Patients wanting least invasive option
4. Biliopancreatic Diversion with Duodenal Switch (BPD/DS)
How it works: Combines sleeve gastrectomy with intestinal bypass
Pros:
Most effective for super obesity (BMI >50)
Highest long-term weight loss (70-80%)
Cons:
Highest complication risk
Requires strict vitamin compliance
Ideal for: Patients with BMI >50 who commit to lifelong follow-up
Comparative Results: Weight Loss Surgery Types
| Procedure | Avg. Excess Weight Loss (1 Yr) | Hospital Stay | Recovery Time | Complication Rate |
|---|---|---|---|---|
| Gastric Sleeve | 60% | 1-2 days | 2-3 weeks | 5-10% |
| Gastric Bypass | 70% | 2-3 days | 3-4 weeks | 10-15% |
| Gastric Band | 40% | Outpatient | 1-2 weeks | 15-20% |
| BPD/DS | 80% | 3-4 days | 4-6 weeks | 15-25% |
Data from ASMBS 2022 Clinical Guidelines (3)
Health Benefits Beyond Weight Loss
Bariatric surgery patients often experience remarkable improvements in obesity-related conditions:
Type 2 Diabetes: 80% achieve remission or significant improvement (4)
Hypertension: 60-70% reduce or eliminate medications
Sleep Apnea: 85% see resolution of symptoms
Joint Pain: 70% report reduced pain and increased mobility
Fertility: PCOS symptoms improve in 90% of women (5)
Potential Risks and Complications
While modern bariatric surgery is safer than ever (mortality rate <0.3%), patients should understand potential risks:
Short-term (≤30 days post-op):
Bleeding (2-4% of cases)
Blood clots (1-2%)
Leaks at surgical connections (1-3%)
Long-term:
Nutritional deficiencies (iron, B12, calcium)
Dumping syndrome (especially with bypass)
Gallstones (30% of patients)
Need for revision surgery (5-10% at 10 years)
The Bariatric Surgery Process: What to Expect
Pre-Op Evaluation (3-6 months)
Medical clearance
Nutritional counseling
Psychological assessment
Surgery Day
Most procedures take 1-3 hours
Typically laparoscopic (small incisions)
1-3 night hospital stay
Recovery Timeline
Return to work: 2-4 weeks
Full recovery: 6-8 weeks
Most weight loss occurs in first year
Life After Surgery: Long-Term Success Factors
Diet:
Progressive stages (liquids → purees → solids)
Focus on protein (60-80g daily)
Avoid sugary/fatty foods
Exercise:
Start walking immediately post-op
Build to 150+ minutes/week
Strength training preserves muscle
Follow-Up Care:
Monthly visits first year
Quarterly years 2-5
Annual visits lifelong
Frequently Asked Questions
Q: How much weight will I lose?
A: Most patients lose:
1 month: 15-20 lbs
6 months: 50-80 lbs
1 year: 70-100+ lbs
Q: Will my insurance cover it?
A: Most plans cover if you meet NIH criteria. Medicare/Medicaid typically approve with proper documentation.
Q: Can the weight come back?
A: About 20% regain significant weight by 5 years, usually due to:
Not following diet
Lack of exercise
Missing follow-ups
Q: Will I need plastic surgery after?
A: About 30% choose body contouring procedures for excess skin after losing 100+ lbs.
Related Frequently Asked Questions
1. What is the minimum weight for bariatric surgery?
Answer:
The minimum weight requirement is based on BMI, not absolute weight. According to the American Society for Metabolic and Bariatric Surgery (ASMBS), candidates typically need:
BMI ≥40 (morbid obesity) or
BMI ≥35 with at least one obesity-related condition (e.g., diabetes, hypertension).
Example: A 5’6” (168 cm) person would need to weigh ≥248 lbs (112 kg) for BMI 40 or ≥217 lbs (98 kg) with comorbidities for BMI 35.
Related: BMI Calculator | Am I a Candidate?
2. Will insurance pay for bariatric surgery?
Answer:
Most private insurers and Medicare/Medicaid cover bariatric surgery if you meet NIH criteria, including:
Documented failed weight loss attempts (e.g., 6+ months of supervised diets).
Psychological evaluation clearance.
BMI/health requirements (see above).
Note: Some plans exclude specific procedures like gastric banding.
Related: Insurance Checklist | Financing Options
3. What is the 30-30 rule for bariatric surgery?
Answer:
The 30-30 rule is a post-op guideline to prevent complications:
30 minutes for meals: Eat slowly to avoid dumping syndrome.
30-minute wait after meals before drinking fluids to prevent pouch stretching.
Why it matters: Violating this rule can cause nausea, vomiting, or weight regain.
Related: Post-Op Diet Guide | Dumping Syndrome Explained
4. What is one of the top 3 causes of death after bariatric surgery?
Answer:
Per a 2023 JAMA Surgery study, the leading causes of mortality within 30 days post-op are:
Pulmonary embolism (blood clots, ~0.1% risk).
Anastomotic leaks (stomach/intestine leaks, 1–2%).
Cardiac events (e.g., heart attack).
Safety note: Mortality rates are lower than gallbladder or hip replacement surgery when performed at accredited centers.
Related: Risks of Bariatric Surgery | Choosing a Surgeon
5. Who gets denied for bariatric surgery?
Answer:
Common reasons for denial include:
Uncontrolled mental health issues (e.g., active eating disorders).
Substance abuse (alcohol/drug dependence).
High surgical risk (severe heart/lung disease).
Inability to commit to lifelong dietary changes.
Appeal tip: Some denials can be overturned with additional medical documentation.
Related: Psychological Evaluation Prep | Appealing Insurance Denials
6. Can you get bariatric surgery at 200 lbs?
Answer:
Possibly, if your BMI meets criteria. For example:
A 5’0” (152 cm) person at 200 lbs has BMI 39 (may qualify with comorbidities).
A 6’0” (183 cm) person at 200 lbs has BMI 27 (does not qualify).
Exception: Some programs offer metabolic surgery for BMI 30–35 with uncontrolled diabetes.
Related: BMI Calculator | Low-BMI Surgery Options
Is Bariatric Surgery Right for You?
While highly effective, bariatric surgery requires lifelong commitment to:
Dietary changes
Vitamin supplementation
Regular exercise
Medical follow-up
The best candidates are:
Motivated to change lifestyle
Free from uncontrolled mental health issues
Committed to long-term care
Next Steps:
Calculate your BMI
Document weight loss attempts
Schedule consultation with bariatric specialist
Citations:
Sjöström L. (2013). New England Journal of Medicine
ASMBS Guidelines (2022)
Aminian A, et al. (2021). JAMA
Arterburn DE, et al. (2020). Diabetes Care
Teitelman M, et al. (2016). Fertility and Sterility
Internal Links: